


Program outcomes
Measured progress that Make the outcomes stick
Licensed admissions · Avg answer time 28s · Private & HIPAA-safe
↓ 62%cravings
Clients reported sustained reduction in urge intensity by week three.
How we do it
- Medication-assisted stabilization when indicated
- Urge surfing + distress tolerance drills
- Trigger mapping and replacement routines
↑ 52%sleep quality
Sleep onset improves and nighttime wakeups drop within two weeks.
How we do it
- CBT-I routines and wind-down stack
- Medication review to reduce sleep disruptors
- Breath pacing and body-based down-shifts
↑ 46%daytime focus
More energy for work, family, and the boring stuff that keeps life stable.
How we do it
- Stimulant/antidepressant optimization when appropriate
- Task chunking and exposure to real-world routines
- Weekly data review and plan adjustments

Real-World Practice, Supervised

| Benefit | Our Program | Typical Program |
|---|---|---|
| Psychiatrist-led dual-diagnosis care (SUD + mental health) | ✓ | Usually Limited |
| Coordination with Primary Doctor | ✓ | Not Always |
| Family Program | ✓ | Not Always |
| Learn Skills You'll Use in Real Life | ✓ | Not Always |
| Client to Staff Ratio | 2:1 | 3:1 or more |
| Medication Assisted Treatment | ✓ | Not Always |
| On-site Detox | ✓ | Not Always |
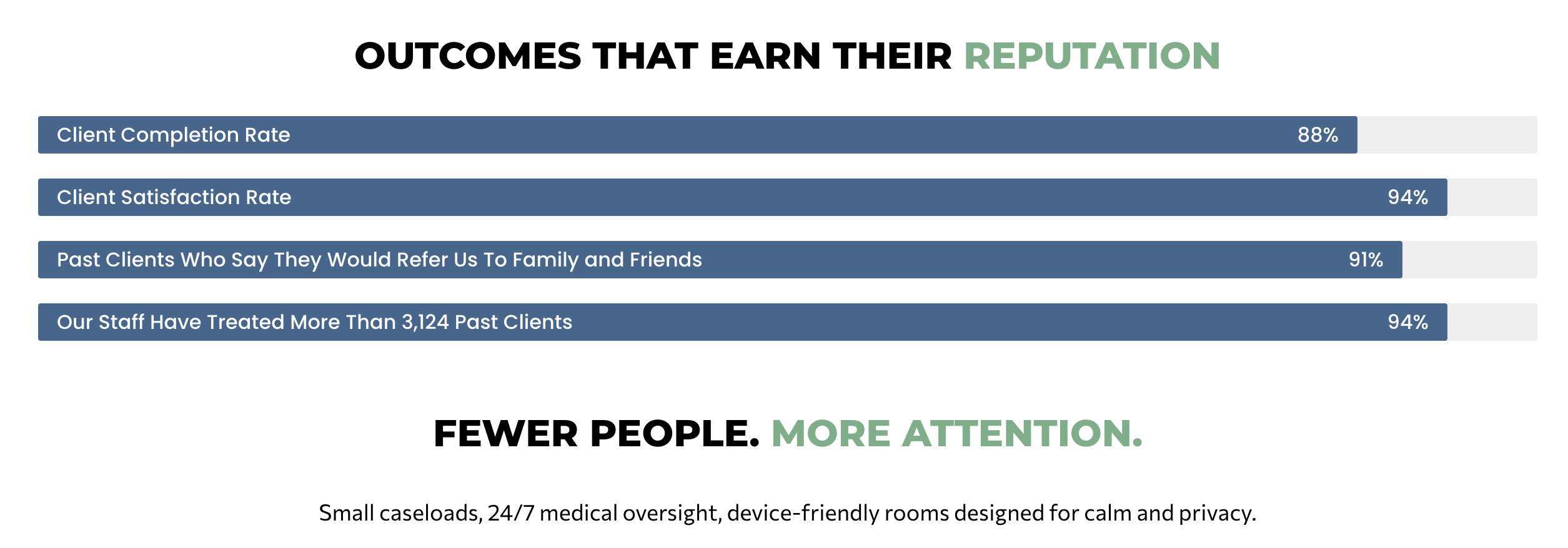
Small caseloads, 24/7 medical oversight, device-friendly rooms designed for calm and privacy.
6 person max
Private rooms
Quiet work areas
Pet friendly
Pool and Jacuzzi
Extended stay

Mental Health, Treated With Medical PRECISION
Integrated, physician-led dual-diagnosis care with outcomes that inform weekly adjustments to your plan.
Psychiatrist on staff
24/7 nursing
Medication management
Trauma-informed
Individual + group therapy
Targeted experiences that reduce cravings, regulate emotion, and help skills transfer to daily life.
Craving regulation
Emotion regulation
Stress tolerance
Social connection

1
Music Therapy
what it does
Guided rhythm, tone and breath syncing to lower arousal and anchor coping routines.
- Craving and anxiety downshift
- Breath + rhythm syncing drills
- Simple home practice between sessions
2
Art Therapy
how it helps
Externalize difficult emotions; build emotion labeling and values clarity without overload.
- Emotion identification and mapping
- Values and motivation work
- Trigger visualization and planning
3
Movement & Breath
why it matters
Low-impact movement and breathwork to reduce physiological drive states that fuel cravings.
- Downshift sympathetic arousal
- Grounding skills for urges
- Sleep prep routines
4
Nature & Community
real-life practice
Supervised outings to practice skills in lower-stress, real-world settings with support.
- Supported exposure and reconnection
- Social skills and confidence rebuild
- Relapse-risk rehearsal with coaching



Targeted experiences that reduce cravings, regulate emotion, and help skills transfer to daily life.
Craving regulation
Emotion regulation
Stress tolerance
Social connection

1
Music Therapy
what it does
Guided rhythm, tone and breath syncing to lower arousal and anchor coping routines.
- Craving and anxiety downshift
- Breath + rhythm syncing drills
- Simple home practice between sessions
2
Art Therapy
how it helps
Externalize difficult emotions; build emotion labeling and values clarity without overload.
- Emotion identification and mapping
- Values and motivation work
- Trigger visualization and planning
3
Movement & Breath
why it matters
Low-impact movement and breathwork to reduce physiological drive states that fuel cravings.
- Downshift sympathetic arousal
- Grounding skills for urges
- Sleep prep routines
4
Nature & Community
real-life practice
Supervised outings to practice skills in lower-stress, real-world settings with support.
- Supported exposure and reconnection
- Social skills and confidence rebuild
- Relapse-risk rehearsal with coaching

Do you accept my insurance?
Most PPO plans are accepted. We’ll verify benefits in minutes and tell you your out-of-pocket before you decide.
No Medicaid/HMO.
How fast can I be admitted?
Same-day admissions are often possible once clinical and coverage checks are complete. We can coordinate travel.
What type of treatment is this?
Measurement-based, evidence-informed care. We track progress regularly and adjust the plan as you improve.
Can you treat mental health and addiction together?
Yes. Psychiatrist-led dual-diagnosis care integrates therapy and medication management.
What happens after I leave?
You depart with a relapse-prevention plan and structured aftercare. Alumni and family support are available.
Will I have privacy and be able to use my phone?
Private rooms are available and devices are allowed.
Can my family be involved?
Yes. We offer weekly family sessions and education so support continues at home.

TALK TO A SPECIALIST and GET A PLAN
IN 7 MINUTES
Confidential. No commitment. Same-day admissions available.
- Private rooms; phones + laptops welcome
- Same-day or scheduled admissions
- Not a match? We'll point you to a better fit.
- We handle travel logistics when needed














